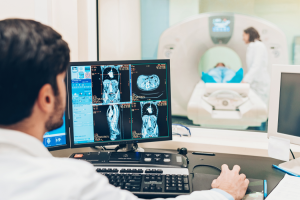
Unlocking Insurance Secrets: How To Get Insurance To Pay For A Tummy Tuck?
Your tummy tuck can be a reality without a hefty price tag! Discover the captivating world of insurance and learn how to make your cosmetic surgery dreams come true without emptying your pockets.
Are you prepared to start a life-transforming journey towards a more confident and slimmer version of yourself? Picture achieving your dream physique without the overwhelming financial burden. It’s not just a wish; it’s a tangible reality.
In this article, we’ll delve into the process of having your insurance cover the expenses of a tummy tuck. We’ll unveil the strategies that can make your dream come true. Tummy tucks can be costly, but by understanding insurance and navigating its intricacies, you may secure financial assistance from your provider.
This article will guide you on how to get insurance to pay for a tummy tuck. We will guide you through each step, offering insights and simplifying the process of getting insurance coverage for your tummy tuck. It’ll make your journey memorable and budget-friendly. Get ready for a voyage filled with possibilities as we explore insurance coverage for your tummy tuck adventure.
How to get insurance to pay for a tummy tuck?
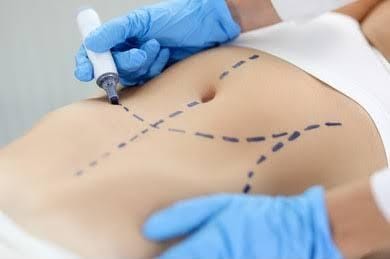
While insurance typically doesn’t cover cosmetic procedures, there are certain scenarios where you can get insurance to pay for a tummy tuck. In this guide, we’ll break down essential information to help you out
- Understand your insurance policy
- Document medical necessity
- Consult with a healthcare provider
- Gather medical records
- Submit a pre-approval request
- Work with experienced healthcare providers
- Follow insurance guidelines
- Be patient and persistent
- Appeal if necessary
- Explore financing options
Understand your insurance policy
Start by thoroughly examining your health insurance policy. Not all policies are the same, and some may have clauses or exceptions that cover specific medical situations. Pay close attention to any mentions of “medically necessary” procedures, as these could be your gateway to tummy tuck coverage.
Document medical necessity
For insurance to consider covering your tummy tuck, you’ll need to prove that it’s medically necessary. This typically involves having a healthcare provider confirm that the procedure is essential for your health, not just for cosmetic purposes. Conditions like excess skin due to weight loss or abdominal muscle separation (diastasis recti) are examples of medical necessity.
Consult with a healthcare provider
Schedule a consultation with a healthcare provider, such as a plastic surgeon or your primary care physician, to discuss your tummy tuck. They can assess your condition and provide documentation to support the medical necessity of the procedure.
Gather medical records
Your healthcare provider may need to compile your medical records, including any tests, photographs, or documented health issues that demonstrate the need for a tummy tuck. This comprehensive documentation will be vital in your case for insurance coverage.
Submit a pre-approval request
Before scheduling your tummy tuck, contact your insurance provider and inquire about their pre-approval process. This step is crucial, as it ensures that your insurance company is aware of your intentions and can offer guidance on their specific requirements for coverage.
Work with experienced healthcare providers
Choose experienced and board-certified healthcare providers for your tummy tuck. Having reputable professionals involved in your care can strengthen your case for insurance coverage.
Follow insurance guidelines
Carefully adhere to any guidelines or requirements set by your insurance company. This includes meeting deductibles, copayments, and other financial obligations.
Be patient and persistent
Getting insurance to pay for a tummy tuck can be a lengthy process. Be patient and persistent in following up with your insurance company and healthcare providers to ensure all necessary documentation is submitted and processed.
Appeal if necessary
If your initial request for coverage is denied, don’t give up. You have the option to appeal the decision. Work closely with your healthcare provider to strengthen your case and provide additional evidence of medical necessity.
Explore financing options
While waiting for insurance approval, explore financing options for your tummy tuck. Some medical facilities offer payment plans or financing to help you cover the costs.
In summary, getting insurance to pay for a tummy tuck involves understanding your policy, proving medical necessity, working closely with healthcare providers, and navigating the insurance process carefully. With persistence and the right documentation, you can increase your chances of securing insurance coverage for your tummy tuck.
Unlocking insurance coverage: Your guide to a flatter tummy
Other than this being included in cosmetic surgery, a tummy tuck surgery is sometimes mandatory to get. We will explore:
- How to get insurance to pay for a tummy tuck after a C-section?
- How to get insurance to pay for panniculectomy?
- How to get insurance to pay for skin removal?
- Securing insurance coverage for a tummy tuck after medical necessity
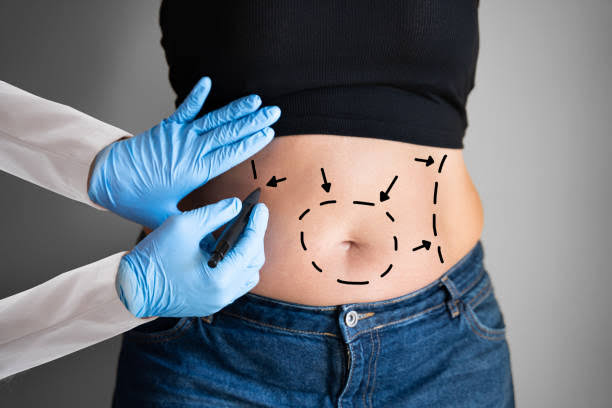
How to get Insurance to pay for a tummy tuck after a C-section?
If you’ve had a C-section and are thinking about a tummy tuck with insurance coverage, you might be wondering how to make it happen. Although it’s not easy, it can be done. Here’s what to do:
Is a tummy tuck after a C-section medically necessary?
The first and most crucial step is to determine if the tummy tuck is medically necessary. A tummy tuck can be deemed necessary if you’re experiencing health issues directly related to the C-section, such as abdominal muscle separation (diastasis recti) or excess skin causing pain or infection.
Consult your doctor
Consult with a board-certified plastic surgeon or your primary care physician. Discuss your reasons for wanting a tummy tuck and any associated health issues. Your doctor’s evaluation and recommendation are essential in establishing medical necessity.
Document medical conditions
Gather all the medical records, photos, and proof that can back up your case. These should include your medical background, any physical or mental health problems from the C-section, and any issues caused by extra skin or muscle separation.
Seek pre-approval
Before setting a surgery date, reach out to your insurance company to learn about their pre-approval process. Find out what documents you need and what to do to improve your chances of getting approval. Don’t forget to keep records of all your talks with the insurance company.
How to get Insurance to pay for a Panniculectomy
A panniculectomy is a surgical procedure to remove excess skin, typically after significant weight loss. Getting insurance to cover this procedure involves the following steps:
Is a Panniculectomy medically necessary?
Start by figuring out if the panniculectomy is medically needed. You have to show that it’s necessary to treat health issues like skin infections, rashes, or problems with your muscles and bones caused by the extra skin.
Consult your doctor
Schedule a consultation with a board-certified plastic surgeon or your primary care physician. Discuss your reasons for wanting a panniculectomy and any associated health issues. Your doctor’s evaluation and recommendation are crucial in establishing medical necessity.
Document medical conditions
Gather all relevant medical records, photographs, and evidence that support your case. This should include documentation of the medical conditions associated with your excess skin, as well as your medical history.
Seek pre-approval
Before scheduling the panniculectomy, contact your insurance provider to inquire about their pre-approval process. Understand what documentation is needed and follow the necessary steps to increase your chances of approval. Keep records of all communications with your insurance company.
How to get insurance to pay for skin removal?
Skin removal surgeries, like panniculectomies and tummy tucks, are often considered cosmetic, but insurance coverage is possible if certain conditions are met:
Is skin removal medically necessary?
You must establish that skin removal is medically necessary. This requires showing that the excess skin is causing health issues such as infections, rashes, or musculoskeletal problems.
Consult your doctor
Consult with a board-certified plastic surgeon or your primary care physician. Discuss your reasons for wanting skin removal and any associated health issues. Your doctor’s evaluation and recommendation are crucial in establishing medical necessity.
Document medical conditions
Gather all relevant medical records, photographs, and evidence that support your case. This should include documentation of the medical conditions associated with your excess skin, as well as your medical history.
Seek pre-approval
Get in touch with your insurance company to ask about how to get approval in advance. Know what paperwork you need and do what’s required to boost your chances of getting a green light.
Securing insurance coverage for a tummy tuck after medical necessity
Getting insurance to cover a tummy tuck, whether it’s after a C-section or for medical reasons, can be tough. Here’s how to deal with it:
Is a tummy tuck medically necessary?
Determine if the tummy tuck is medically necessary. It must be shown that the procedure is required to treat health conditions, such as abdominal muscle separation (diastasis recti) or excess skin causing pain or infection.
Consult your doctor
Your doctor’s evaluation and recommendation are crucial in establishing medical necessity. Ensure to consult a plastic surgeon who is board-certified with relevant experience. Research their work if you have to.
Document medical conditions
Collect all your important medical documents, pictures, and proof that back up your situation. This should cover records of the health issues linked to your tummy tuck necessity and your medical background.
Seek pre-approval
Reach out to your insurance company to learn about how to get pre-approval. Figure out what paperwork they require, and make sure to follow the right procedures to boost your approval odds. Remember to keep a record of all your interactions with the insurance company.
How to get health insurance to pay for tummy tuck: Insurance roadmap decoded
Here’s how to get health insurance to pay for a tummy tuck. We will navigate:
- How to get your insurance to cover a tummy tuck?
- How to get Medicaid to pay for tummy tuck?
- How to get Tricare to pay for a tummy tuck?
How to get Medicaid to pay for a tummy tuck?

Here’s is what you should do:
- First, discuss your tummy tuck with your doctor and make sure it’s deemed medically necessary.
- Gather medical records that support the need for the procedure, especially if it’s due to health issues like infections or rashes.
- Get in touch with your local Medicaid office and inquire about their tummy tuck coverage policies.
- Learn about their pre-approval process, as it may vary by state, and follow their requirements closely.
- Keep a record of all conversations and correspondence with Medicaid for future reference.
How to get Tricare to pay for a tummy tuck?
Here is what you should do:
- Ensure that the tummy tuck is necessary to address specific medical conditions.
- Collect evidence such as medical records, photos, and information about health issues caused or worsened by excess skin or muscle separation.
- Reach out to Tricare, the military healthcare program, to understand their tummy tuck coverage policies.
- Get details on their pre-approval process, which may have specific requirements for military beneficiaries.
- Keep records of all interactions with Tricare, including names, dates, and details of discussions.
How to get health insurance to pay for a tummy tuck?
Here is what you should do:
- Ensure that your tummy tuck is medically necessary, often due to health issues like infections, rashes, or musculoskeletal problems.
- Gather all relevant medical records, photographs, and proof that support your case.
- Get in touch with your health insurance company to inquire about tummy tuck coverage.
- Understand the pre-approval process of your insurance company, which may include specific requirements or forms.
- Maintain a detailed record of all interactions with your insurance provider, including who you spoke with and what was discussed.
These specific requirements and coverage can vary based on your insurance plan, so always consult with your healthcare provider and insurance company to ensure you follow their specific rules and procedures.

FAQs
Q1: Can I get insurance coverage for a tummy tuck after a C-section?
Yes, if the excess skin from a C-section leads to medical issues, it may be considered for insurance coverage.
Q2: What role does my chosen surgeon play in the insurance process?
Your surgeon can assist with necessary documentation and may provide additional information to support your case.
Q3: What are some insurance companies’ specific requirements for tummy tuck coverage?
Specific requirements can vary by insurance provider, so contact your insurer for details on their criteria.
Q4: Can I receive insurance coverage for a tummy tuck with Tricare, the military healthcare program?
Tricare may provide coverage for a tummy tuck if it’s deemed medically necessary. Contact them for details on their policies.
Q5: What if my tummy tuck is not deemed medically necessary?
If a tummy tuck is considered elective, cosmetic, and not medically necessary, insurance coverage is unlikely.
Q6: Can I appeal a denied insurance claim for a tummy tuck multiple times?
Yes, you can appeal more than once if your initial appeal is denied, providing further information and documentation as needed.
Q7: How long does it typically take to get insurance approval for a medically necessary tummy tuck?
The timeline can vary, but insurance processes can take several weeks to months, so patience is essential.
Insurance coverage for a tummy tuck is often limited to medically necessary cases. To explore this option, consult with your insurer and surgeon, providing the required medical evidence. If insurance doesn’t cover it, don’t lose hope. Other financing avenues, such as personal loans and payment plans, can make your dream of a tummy tuck a reality. Remember, your journey to a transformed, confident you are just a step away!