Which Insurance Covers IVF?
Undergoing fertility treatment can be emotionally and financially draining, and suitable fertility insurance can remove some of the stress. This article will cover some of the best IVF insurances.
As per the Centers for Disease Control (CDC), infertility is a typical problem. Around 9% of men and 11% of women of reproductive age in the United States have had fertility problems. Most of these situations have led the couple to go for an IVF. So which insurance covers IVF? Fertility insurance covers the diagnosis, procedures, and treatments required to assist parents-to-be who find it difficult to conceive or carry a child to term. Fertility insurance is not generally a separate health insurance policy. However, numerous health insurance providers cover it under health care plans. Presently, seventeen states have laws that make it mandatory for health insurance providers to cover fertility treatments. Nevertheless, since it is not necessitated in all states, not all insurers cover treatments, and some might cover a limited number of treatments or only specific types of treatments.
Need for In Vitro Fertilization (IVF) treatment

IVF helps infertile who desire to have a child. Due to the cost and invasiveness of IVF, many couples first attempt alternative reproductive therapies. These might involve intrauterine insemination or using fertility medications. In such an operation, sperm is directly injected into a woman’s uterus by a medical professional.
Issues with infertility for which It may require IVF include:
- Reduction in fertility in women over 40
- Damaged and blocked fallopian tubes
- Endometriosis
- Uterine fibroids
- Decreased ovarian function
- Male infertility, such as unexplained infertility, low sperm count, or sperm quality problems.
If they face the danger of spreading a genetic condition to their children, parents may also choose IVF. The embryos can be examined for genetic abnormalities in a medical laboratory. Only then are embryos without genetic flaws implanted.
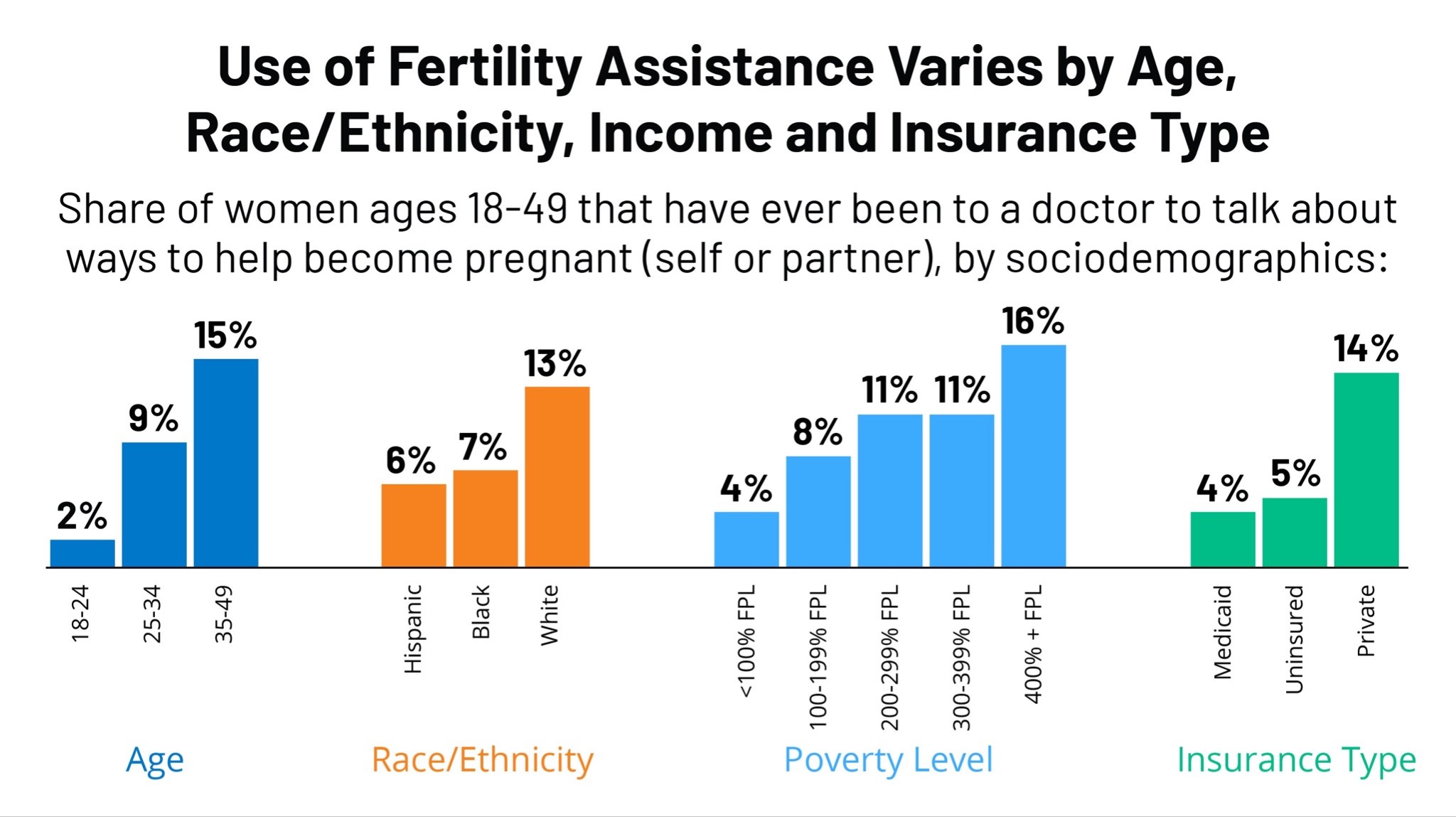
The graphical representation of how many females are searching to become pregnant to age, race/ethnicity, income, and insurance follow.
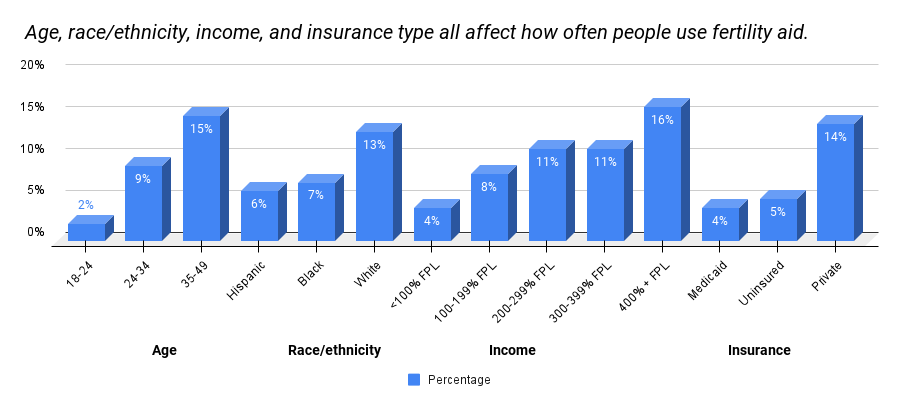
How to get IVF covered by insurance?

Ask your employer for benefits
If your company does not already provide fertility insurance that covers IVF, directly asking for it may seem like a bold step. However, certain employers take the advice of their insurance brokers. They need to find out if they can ask brokers to add coverage for fertility treatment. They can ask their broker to:
- Give their employees two health plans: one that provides the benefit of IVF and another that does not.
- Look for an IVF rider to benefit from adding to their current plan.
- Replace an employee’s plan with one that gives IVF benefits.

Do not hesitate before telling your employer that you need IVF insurance. In some situations, employers need to hear from their employees.
- Employers are either self-insured (insurance organizations handle the benefits, but the employer covers the claims) or fully insured (insurance organizations take benefits and cover the shares). Self-insured employers are determined to offer IVF coverage after they learn the cost savings associated with providing help.
- Employers must be competitive and want to know other organizations’ coverage and benefits packages.
- If more employees contact their Human Resource Departments, employers will better comprehend the need for IVF insurance. Moreover, they would make sure that there is no limitation to the range of coverage provided.
- You know the employer will know that there is a need for IVF coverage.
With adequate infertility benefits, patients tend to transfer fewer embryos in an IVF cycle. The healthcare cost of a singleton pregnancy (through birth) is estimated at $21,458. For twins, it is around $104,831; for triplets, it is approximately $407,199. There are also savings in mental health benefits. When employers are told this could apply to 1 in 6 employees, they consider it more seriously.
Ask your insurer for coverage
While requesting coverage, your story will make your request for extra advantages (an Exemption of Benefits or Predetermination of Coverage) memorable. With a letter from your primary care physician and additional examination:
- You should attempt to persuade the insurance organization that you are a good investment with a reasonable possibility of success (you have more than a 5% chance of live birth)
- Have a clinical requirement (IVF is your only choice) and can save them cash (patients with IVF benefits have more singleton births).
These reasons will help legitimize making a mutually beneficial solution for everybody.
Numerous individuals think the insurance inclusion they offer needs to be improved. However, you can request special consideration. The objective is to simplify the insurance medical director’s work to abolish the organization’s policy and provide you with benefits. You can remind the insurance provider that IVF benefits give access to cheaper health care, which empowers patients to choose their treatment based on medical recommendations instead of financial concerns.
You can share research showing that patients generally transfer multiple embryos without insurance benefits, increasing the odds of high-risk pregnancies and premature births. There are quotes from insurance organization medical directors who define a clear boundary between insurance providers offering IVF benefits and significant savings on the maternity and neonatal side. It can look these facts up on Google or within The Policymaker’s Guide to Fertility Health Benefits.
Purchase non-group insurance
You can find non-group insurance or a non-group plan (or individual plan not offered through an employer) that gives IVF benefits. These plans have a heavy monthly premium. However, it is way less than paying out-of-pocket for a complete IVF cycle. So remember that such programs do exist. States have assigned companies or an insurance department to assist shoppers with exploring the available insurance plans to determine which one will work best. To find out your state resources, you can search for “organization to find a health insurance plan (name of state)” and “(name of state) insurance department.” You can do a quick online search for the insurance branch of each state. Usually, you can apply for these plans if there has been a significant change in your life (business, family, and so on) or during a yearly open enrollment period.
Participate in clinical research trials

Applying for a fertility clinic research spot is another alternative to paying for treatment. Fertility centers often look for patients for clinical preliminaries. The treatments and discounts offered by centers can change. You can look online or visit websites like centerwatch.com or clinicaltrials.gov to discover preliminaries by condition and area. Once you have found a research trial that intrigues you, you need to apply. If you are selected to participate, read the agreement’s fine print. Before signing up, you must ensure you get your responsibilities and what the clinic offers. Those taking an interest get a considerable advantage while helping advance health care.
Seek employment from a company that provides infertility coverage

A few people assume they will be guaranteed insurance coverage if they live in a state with an infertility mandate. While some states require completely insured employers to give IVF inclusion, self-insured businesses can choose not to offer this advantage. What makes a difference is the state where the employers’ headquarters are found and which organizations give insurance benefits.
For instance, suppose you live in Arizona, a state without mandated advantages, and work for CVS. CVS has its headquarters in a state with a law requiring IVF benefits, which implies that you will have benefits even though you live in Arizona. Fortunately, numerous organizations offer advantages, from retail (TJ Maxx) and banking (Bank of America) to technology (Apple). In principle, everybody should have the option to get a job where they can apply their range of abilities in an organization that provides benefits.
Not all organizations offer a similar range of advantages. One organization may intentionally give $15,000 in inclusion to use toward IVF, while others might contribute $4,000 or up to six IVF cycles. Often you can gather extensive data on which benefits various employers offer by participating in online forums and looking over your local community. It can find discussions on Facebook or other online networks. In case you are not able to find a full-time occupation with IVF inclusion, you can apply for a part-time job where it is offered. Pregnantish has featured the story of Christian Borrero-Colon, a US serviceman who accepted a position with Starbucks only to get infertility insurance coverage.
Uses Of Fertility Insurance
Many people struggle to become pregnant without help and require fertility treatments. The need for such therapies could be because of infertility or because the person is in a same-sex or single relationship. Fertility insurance covers the cost of conceiving a child for individuals who cannot do so naturally. Fertility insurance coverage is precisely based on the individual policy and the location. Coverage may include the following treatments:
Diagnostic Services |
● Lab Tests (e.g., progesterone, ovarian reserve, thyroid studies, prolactin)
● Semen Analysis ● Imaging (e.g., pelvic ultrasound, hysterosalpingogram (HSG)) ● Diagnostic procedures (e.g., Laparoscopy, Hysteroscopy) |
Treatment Services |
● Medications (e.g., Clomid/clomiphene citrate)
● Surgery (e.g., Laparoscopy, Hysteroscopy) ● Intrauterine insemination (IUI) [also known as “artificial insemination”] ● In vitro fertilization (IVF) [a type of assisted reproductive therapy (ART)] |
Fertility Preservation |
● Cryopreservation [also known as egg/sperm/embryo “freezing”] |
The fertility insurance laws are complex and may be unique to a specific state. For instance, insurers who give maternity benefits in Utah must also provide adoption and infertility treatment services. In Minnesota, fertility drugs mainly used to boost fertility are not covered. People looking for fertility insurance coverage should thoroughly know the state laws in their area and the individual company’s range.
Are there any services that fertility insurance does not provide coverage for?
Fertility insurance coverage varies depending on the state and its regulations. Currently, nineteen states have enacted laws mandating fertility insurance inclusion, including Arkansas, California, Colorado, and others.
While most states cover IVF treatment, some, such as California, Louisiana, and Texas, typically exclude IVF, ICSI, and ZIFT. It’s important to note that coverage might extend to diagnosis but not treatment of infertility.
Even in states with IVF coverage, cryopreservation and embryo storage may still be excluded. Additionally, regardless of location, services involving sperm or egg donors, surrogacy, and reversal of voluntary sterilization are commonly excluded from policies.
Does any insurance company cover IVF?
UnitedHealthcare

UnitedHealthcare provides affordable health care coverage via a broad network of care providers in 50 states that, based on your condition and plan, includes fertility insurance. This organization offers inclusion for things like ovulation induction (for women up to the age of 44), insemination procedures, artificial insemination, intrauterine insemination, and assisted reproductive technologies. All required treatments in states that require specific fertility coverages are covered. Certain therapies, like paying for donor eggs and sperm and long-term sperm, egg, or embryo storage, are excluded.
UnitedHealthcare has a network of over 1.3 million medical providers and 6,500 medical facilities. Your plan expenses, deductible, and copay options will be based on your plan, your state, and the level of coverage you choose. The provider usually pays around 80% in cost-sharing programs, which implies that you would have to pay for 20% of covered fertility services. UnitedHealthcare allows you to handle your care and payments through a smartphone application, making it easier to connect with fertility specialists. A well-respected insurer, UnitedHealthcare was established in 1977 and 2020; AM Best gave it a financial strength rating of A-.
Cigna

Through many of its plans, Cigna offers a comprehensive exhibit of assisted reproductive technology coverage, including IVF. Moreover, it gives scope for diagnostic tests like hysteroscopies, semen analysis, and testicular biopsy. Fertility treatments like ovarian reserve testing, tubal recanalization, assisted embryo hatching, intrafallopian gamete transfer, and testicular therapies and surgeries are usually approved techniques.
Cigna offers individuals a vast network of suppliers and has a smartphone application to assist individuals with handling their care. Medicare, group, and individual and family plans through the health care insurance marketplace are offered in 10 states (Arizona, Colorado, Florida, Illinois, Kansas, Missouri, North Carolina, Tennessee, Utah, and Virginia). Your deductible and fertility coverage qualification will depend on your plan and state. Established in 1981, Cigna has gained notoriety for giving comprehensive care at an affordable cost. AM Best, as of now, rates them A for their financial strength and claims-paying ability.
Aetna

Its broad online library of tools, recordings, and resources around infertility will assist you with learning about fertility care and how to get to it. While Aetna’s plans vary on what they cover, if your plan covers infertility, you can get treatment for things like diagnostic tests, including physical exams and treatments like in vitro fertilization, assisted reproductive technologies, and artificial insemination. They exclude individuals trying to get pregnant at over 40 years of age from some of their fertility healthcare.
Aetna’s rating system distinguishes a few fertility care offices as Institutes of Excellence (IOE). It is a regional network of facilities and suppliers with an extraordinary history of providing fertility care with positive outcomes. Aetna’s network has 1.2 million health care experts, more than 690,000 doctors and specialists, and more than 5,700 facilities.
Aetna does not offer individual and family plans on the healthcare coverage marketplace. They just provide Medicare, Medicaid, and employer-sponsored plans. These plans incorporate HMO, PPO, POS, EPO, and HDHP plans, where your deductible and copays vary by program. They have an application that assists you with handling your care to make exploring your coverage simpler. Established in 1852 and headquartered in Hartford, Connecticut, Aetna works in 50 states and Washington, D.C. The organization got an A rating from AM Best in the financial strength category.
Wellcare

Wellcare offers Medicaid and Medicare coverage that also incorporates some fertility coverage. Its range supports individuals who experience infertility between the ages of 21 and 44. They cover essential infertility services like semen analysis, endometrial biopsy, treatment of ovulatory dysfunction, and testis biopsies. They also cover comprehensive infertility services like pelvic ultrasounds, laparotomy, and artificial insemination. They do not cover things like in vitro fertilization, donor ovum or donor sperm, storage expenses, or reversals of vasectomies.
Wellcare has a network of more than 571,000 healthcare experts they work with nationwide. They sell plans in each of the 50 states, and your plan premium and deductible will vary contingent on your condition and the arrangement you pick. They have a smartphone application to assist you with handling your care. Established in 1985, Wellcare is known for giving excellent care to its individuals. The National Committee for Quality Assurance (NCQA), an accreditation association that rates health plans, gave WellCare a rating of 2.5 to 3.5 out of 5.0 in 2020.
Progyny

They give the most comprehensive and premium coverage of any plan. An independent policy to assist employees with their fertility battles, Progyny gives benefit bundles to employers who want to select and keep employees with appealing fertility coverage. Progyny is a good plan since its methodology centers around results rather than diminishing expenses. Numerous health plans start with cheaper procedures, yet Progyny permits its patients and their PCPs to choose. The best treatment strategy is to give them access to the assisted reproductive technologies they need to conceive and have a kid without proving that cheaper treatments do not work.
Each member requiring fertility treatment is allotted their own Patient Care Advocate who assists them with organizing appointments, offers emotional help, and answers their treatment questions. The plan often incorporates medicines for fertility treatment with next-day medication delivery. Progeny works with more than 900 fertility suppliers at more than 650 offices nationwide, the most significant national fertility network for a supplier. They additionally offer custom application support to assist you with learning more about fertility and handling your mental and emotional health during your fertility venture. Established in 2008, Progyny is a recent addition to the fertility insurance market. However, it gives a customized fertility experience to those whose employers offer the arrangement. Conspicuous organizations offering Progyny’s services as advantages incorporate Google and Apple.
Which healthcare plans cover IVF?
UnitedHealthcare
- Policy Types: HMO, HMO-POS, PFFS, PDP, D-SNP, PPO, EPO, POS, HDHP
- Coverage Limit: Not stated online
- States Available: 50 states
Cigna
- Policy Types: HMO, PPO, EPO, POS, SNP, PDP
- Coverage Limit: Not stated online
- States Available: 10 states
Aetna
- Policy Types: HMO, PPO, POS, EPO, HDHP
- Coverage Limit: Not stated online
- States Available: 50 states and Washington, C.
Wellcare
- Policy Types: HMO, PPO, PFFS, D-SNP, C-SNP, PDP
- Coverage Limit: Not stated online
- States Available: 50 states
Progyny
- Policy Types: 1
- Coverage Limit: No stated limit
- States Available: 50 states
Which state covers IVF insurance?

Since the 1980s, 17 states — Arkansas, California, Connecticut, Delaware, Hawaii, Illinois, Louisiana, Maryland, Massachusetts, Montana, New Hampshire, New Jersey, New York, Ohio, Rhode Island, Texas, and West Virginia — have passed laws that expect insurance providers to cover or offer coverage for infertility diagnosis and treatment. Of those states, 15 have laws requiring insurance agencies to cover infertility treatment, and two states — California and Texas — have laws requiring insurance agencies to bring coverage for infertility treatment to the table.
Why is IVF not covered by insurance?
In states with no infertility coverage command, most insurance plans only assist a little with payment for fertility and IVF services. IVF insurance coverage is more uncommon than coverage for fertility benefits other than IVF. It is because IVF costs more than additional infertility testing and treatments. Even though fertility treatments are costly, more normal healthcare plans are beginning to cover them. One reason for this is that 17 states have now made it necessary for fertility treatments to be covered. More states are also moving to administer fertility coverage. In states that do not have these commands, you may have to take a more costly approach to get fertility treatments covered. The amount you will pay differs significantly, yet it is commonly more affordable than paying for out-of-pocket fertility treatments since only one IVF cycle costs an average of $12,000. Numerous individuals who do not have coverage take out an IVF loan to take care of the expenses.
How much does fertility insurance cost?
Fertility insurance goes under the umbrella of general health care insurance strategies. There will be related expenses if you need to enroll in a health plan.
| Monthly premiums for healthcare coverage | $300 |
| The entire range of healthcare coverage | $2000 |
You must pay the expense when you attend an appointment for covered fertility services. It can be a fixed copay amount, for example, $25 for a doctor’s visit, or coins, rance, a percentage of the total, commonly around 20%. Every year you should pay a specific amount of cash before the medical coverage starts to pay. This is known as the deductible. Some insurance policies, particularly the more expensive ones, may have a zero deductible. With the essential guidelines, you might be expected to pay around $7,000 before the coverage starts.
The costs associated with infertility treatment are staggeringly variable and can be costly, contingent upon the services required. Thus, numerous insurance providers only give coverage if necessary. The Kaiser Family Foundation states that the average cost for effective IVF treatment with a donor egg could cost more than $72,000. In comparison, IUI is considerably less expensive at around $300 to $1,000 without insurance. Due to the high expenses included, carefully check your cost-sharing sum in the policy documentation.
FAQ
What age is ideal for IVF?
Women in their 20s and early 30s who undergo IVF have the most significant success rates. Once she enters her mid-30s, the success rates start progressively declining.
Which situation did IVF require?
IVF is used to assist in a woman’s pregnancy. It is used to treat various infertility issues. One of them is advanced maternal age (progressive woman’s age), Fallopian tubes that are damaged or clogged (which might be brought on by pelvic inflammatory illness or previous reproductive surgery).
Who is unsuitable for IVF?
Underlying health issues- specific medical problems may significantly impact your ability to conceive or sustain a healthy pregnancy. These disorders such as endometriosis, polycystic ovary syndrome (PCOS), and premature ovarian failure.
How do IUIs and IVF differ?
The main difference between IUI and IVF is that internal fertilization occurs with IUI. In other words, the sperm is injected directly into the woman’s uterus. So that the fertilization is successful, the embryo will also implant there. When using IVF, fertilization occurs in a lab, externally or outside of the uterus.
Conclusion
Fertility insurance typically integrates into individual, family, group, or government-sponsored health plans. However, when obtaining an individual or family health plan through the health insurance marketplace, one can specifically select coverage inclusive of fertility services. Some individuals seeking fertility coverage opt for separate private health insurance policies via the health insurance marketplace, augmenting their existing employer-offered health coverage with enhanced fertility treatment benefits. Additionally, certain employers extend fertility-only coverage as part of their benefits package, although these are not available to individuals. Navigating the landscape of health insurance for fertility treatments can be time-consuming and bewildering. Coverage strategies vary according to state laws, and even providers extending coverage might limit it to diagnosing fertility issues rather than offering comprehensive treatment solutions.






